Learning from best practices, drawing lessons from other parts of the world and incorporating them into one’s mode of operations is good.
This cuts across individuals, firms and countries. It also applies in all sectors of the economy- from education, finance, agriculture and so on. The picture is no different in health.
More importantly, it appears when a developing country adopts a model from a developed one, then it shows the former is on the right track. But, the bigger question is whether the adopting country has considered all factors to determine if indeed it is making the right choice that will holistically inure to the benefit of its citizens.
One of the building blocks of a country’s health system is its service delivery. This is essentially so because patients need to enjoy a minimum quality of standardized service while securing easy geographical, financial and equitable access.
It is against this backdrop that successive governments in Ghana continuously restructure health service delivery to adjust to modern standards. The Ministry of Health together with the Ghana Health Service (GHS) has over the years made reforms and rolled out interventions aimed at meeting the health needs of the ordinary Ghanaian at the basic level. But one policy that has recently been introduced which does not sit well with me is the one for ‘drone for emergency medical supplies’.
The drones will start work according to government later this month, April.
I was fascinated when I heard about the innovation making its way to Ghana. I wondered why such a plan was coming into force when many of our health intervention programs particularly the Community-based Health Planning and Services (CHPS) continue to suffer just because of poor management.
CHPS, according to the GHS, is a national strategy to deliver essential community -based health services involving health planning and service delivery with the communities. Its primary focus is communities in deprived sub-districts and bringing health services close to the communities.
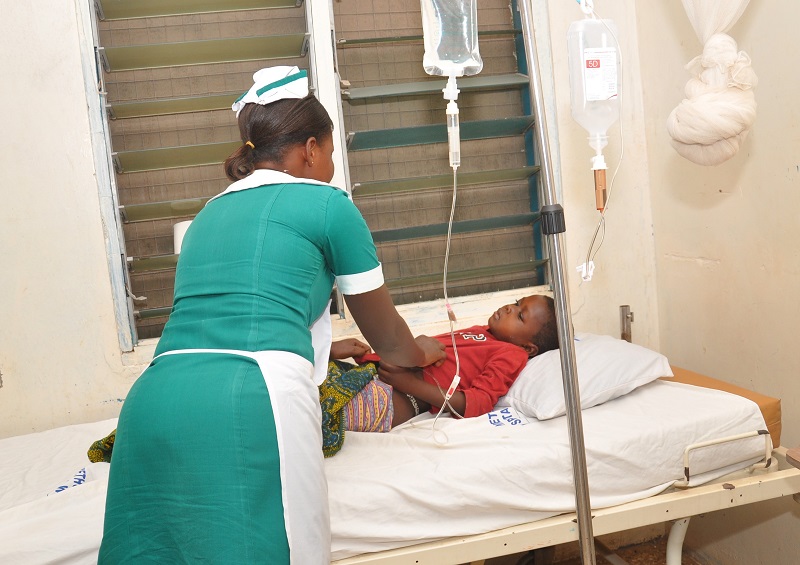
The idea was to set up a health facility within a certain radius to cater for the basic or primary health needs of the people. So a building is put up with all the basic requirements of a healthcare facility including a simple laboratory. A room is made available for the Community Health Nurse or Officer in the compound as accommodation. This is to ensure that at every time of the day or night, the health officer is available and accessible to the community. They do not have to travel long distances over a snake bite or simple malaria or a small cut. The CHPS would also provide health education and immunization services to the community.
For a developing country like Ghana where geographical access to healthcare continues to be a major challenge, it is not out of place for authorities to find innovative ways of bringing healthcare to the doorstep of citizens. But for the over two decades since the CHPS initiative was introduced in Ghana, its operationalization has been saddled with nothing but inefficiencies. And for us to introduce another innovation – that is of no pressing significance now – that may take the life out of an already struggling program, for me is disturbing.

A proponent of the drone deal, Dr. Thomas Mensah (inventor and father of fibre optics) insists, “Small commercial drones will deliver emergency services to remote villages and small clinics to receive medicines, blood since there are no helicopters to travel to these remote areas.” This seems workable in principle. In any case, it makes sense if there is a vaccine shortage at the Tema General Hospital, clinicians there make a request from the Korle-Bu Teaching Hospital and receive the supplies in about 15-30 minutes to save a life. After all, some other countries are practising telemedicine.
But what happens really in the remotest part of the country where these ‘small clinics’ are? In some cases, there may be no single health facility or even if there is, it lacks health personnel and even if there are, no proper equipment is available. Does it solve any health needs in the rural areas both government and its agencies use in defence of the policy?
Ghana is paying approximately $12 million in this deal which is expected to distribute health supplies to under-served areas in the country for four years at an operational cost of $88,000 per month for each of the four distribution centres. For every single delivery, operators of the drones – Zipline will charge $17. Are we saying the final consumer will not have his part of the cost burden? The argument has been that this is a stop-gap measure to assist health centres in dire need of medical aid. It is cost effective and chances are that Ghana becomes the first in the West African sub-region, the second after Rwanda in Africa and the largest in the world to use this advanced technology.

In analyzing the cost benefits, many may argue that the overall cost of the deal will not even be sufficient to cater for other health expenditure within the short to medium term. Whatever it may be, did government not lose its scale of preference? The amount spent for this if not fully, should be able to cater for some basic necessities for our primary health care facilities. At least, the operational cost of the drone deal can construct and or equip some CHPS compounds to expand the coverage of health service because of the low-cost.
What makes my heart bleed is the sustainability of the deal. I am not spelling doom for the project but I doubt if it will be well maintained judging from other ‘failed’ health policies we have managed. Are we prepared for its proper monitoring and evaluation? Will the government be able to meet all payment requirements on time to avoid breaches and possible termination of the deal as specified in the contract document. Will the opposition party abrogate the contract should they come into power which will cost the country huge sums of money? Do nurses and doctors and general hospital staff who are already overburdened with other duties have the capacity to handle the drone deliverable assuming they even get there?
Over the years, it became necessary that CHPS be introduced as a community-based care provider. It was more or less the decentralized form of healthcare delivery due to the fact that basic and essential health care services were not finding their way to the length and breadth of the country.
Today, what was considered to be a strategy to provide universal health coverage at the primary stage is near a charade. Fundamentally, the underlying principle for which it was established has fallen off. Efforts to get community involvement through volunteerism are not forthcoming. Mobilization of capital and human resources is almost impossible. Existing compounds are finding it extremely difficult to perform basic services such as child welfare clinic, family planning, basic consulting and provision of some essential drugs. Attempts to even get more of such facilities are moving at a rather slow pace. The sick is resorting to self-medication because the payment for healthcare continues to be a toll on many Ghanaians, as funds due the CHPS do not come regularly.

The construction of some health facilities have grounded to a halt. Clients on the National Health Insurance Scheme are struggling because the program is taking a nose dive. There seems to be no solution for the deadly ‘No Bed Syndrome’. How far have we come good with our National Blood Bank? Trained health professionals are not accepting posting to rural communities over lack of incentives. These are just a few of the myriad of challenges facing our health sector. Yet, we do not consider strengthening if not all, any of these before settling for something entirely new?
Sustainable Development Goal (SDG 3) requires that countries ensure healthy lives and promote wellbeing for all at all ages. How does Ghana achieve this when it is paying less attention to the very reason the CHPS initiative was introduced and for that matter, its primary health care system. Goal (3c) specifically speaks to it more.
It says “substantially increase health financing and the recruitment, development, training and retention of the health workforce in developing countries, especially in the least developed countries and Small Island Developing States”. Is Ghana close to any of these as we look forward to 2030? The 2019 World Health Day nails it right on the head when it was celebrated under the theme, “-Universal Health Coverage: everyone, everywhere.”
I heaved a sigh of relief when Members of Parliament who passed this drone deal admitted that the inadequacy of CHPS compounds was impeding Ghana’s Universal Health Coverage aspirations.

Ghana has not been able to achieve Universal Health Coverage partly because health inequalities still exist, and this very disproportionate access to health is increasing. Communities are still not seeing the development they so deserve, health facilities are still far apart in rural areas. Inadequate staffing coupled with the brain drain in the health sector is also not ending anytime soon. It must be admitted that enough resources have not been committed to expanding the CHPS program. How did we get here with the drone plan? Political actors must also have their share of the blame because no proper research is conducted to guide policy development and implementation. This seeming lack of evidence-based health reforms is problematic.
Whilst we cannot rule out Comparative Health Systems for anything, no country can also neglect its primary health care system. But it does not mean that if Rwanda has settled for drones, we should do same. We may simply not be there yet or our context may be different. If this is not the case, then we can equally adopt the ‘bare-foot doctors’ system in Cuba and stop seeking the services of Cuban doctors in Ghana. We can equally commit resources and improve our traditional and herbal health regime just like China. Do these not fit perfectly for Ghana?
First things first! Many barriers to accessing healthcare in Ghana have not yet been broken. The drone for medical supplies is a no go area when our CHPS compounds which serve as the first point of call in health care delivery continue to be in their dilapidated state.
–
Written by: Nii Larte Lartey | nlartelartey@gmail.com
The author is a National Service Personnel with Citi FM / Citi TV. Nii Larte has an interest in issues that centre on Health, Education and Young people.