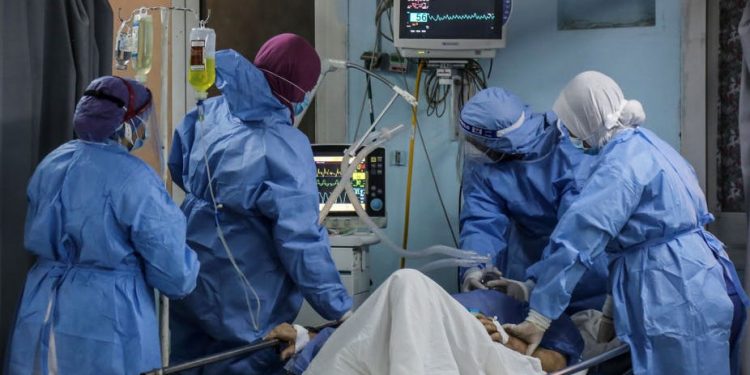
In March 2020, those of us living on the African continent were terrified about what would happen. We had watched Wuhan and then Italy get overrun by Covid-19. These were environments far more resourced than Africa.
We knew that we had a limited healthcare workforce. And we have estimated that there was about one critical care bed per 100 000 population on the continent. The average across Europe was over 11 per 100 000 population.
What scared us even more was a lack of information about how to manage critically ill Covid-19 patients in resource limited environments. Steps were immediately taken to fill this void. The African Perioperative Research Group, an African research network, rapidly pivoted to conduct a continental study to determine resource, clinical factors and therapies associated with mortality or survival in critically ill patients.
The interim analysis was disseminated in a preprint last year to help healthcare providers. Now the full study of over 3000 critical care Covid-19 patients from 64 hospitals in 10 African countries has just been published.
The picture it paints is bleak. It shows that there have been excess deaths following Covid-19 critical care admission in Africa compared with the global average. And that the mortality of critically ill Covid-19 patients in Africa exceeded that of any other region in the world.
The bad news doesn’t end there. For every two Covid-19 patients referred for critical care treatment, only one was admitted to a high or intensive care unit. These patients in Africa have an excess mortality of between 11 and 23 extra deaths per 100 critical care admissions in Africa when compared to the global average. The mortality in Africa is 48.2%.
We suspect that these grim data probably provide an optimistic estimate of critical care outcomes on the continent. It is likely that the participating sites were relatively more resourced than other non-participating critical care units in Africa. Unfortunately, these data confirmed our fears when we set out on this project. Saving lives of critically ill Covid-19 patients in Africa is difficult for various reasons.
The grim reality
Our results show that even simple monitoring of patients was not universally available. One in ten hospitals could not provide pulse oximetry to measure arterial blood saturation to all critical care patients. Arterial desaturation is an important sign of a failure to adequately manage a severe respiratory disease such as Covid-19.
Pulse oximetry would be considered a basic requirement in critical care, and inadequate monitoring results in a delay to respond to deterioration. A delay in response is associated with mortality.
Secondly, there was insufficient equipment to provide advanced care at the participating sites. As a result, the ability to provide interventions (such as dialysis and proning (placing patients on their tummies)) was estimated to be delivered between seven and 14 times fewer than what would be expected for these patients based on the severity of their illness.
A commentary on our study also suggested caution when counting available equipment in Africa. It is well documented across Africa that a substantial amount of equipment doesn’t work. This is often because it has been donated and is not appropriate for the environment. There are also often no service contracts to maintain it.
The reality about scarce resources is that once a patient in the critical care unit is being given a particular therapy, such as dialysis, it is then unavailable to the other patients while in use.
These factors certainly would result in excess mortality.
Besides known risk factors for mortality in severe Covid-19 infection, our study also showed that HIV/AIDS was associated with an increased risk for mortality.
Finally, our findings confirmed that steroids are associated with survival benefit in our patients, consistent with the (RECOVERY) (Randomized Evaluation of Covid-19 Therapy) trial. Steroid therapy decreases the inflammatory response contributing to the severity of the illness. That’s why it’s essential that it’s readily available for critically ill Covid-19 patients.
Urgent next steps
This study has two important implications for policymakers.
Firstly, there is the immediate response. It is critical that vaccination is made a priority. Vaccination is an important intervention when it is impossible to provide safe and adequate critical care across the continent.
Vaccine inequality cannot be accepted, and it is important to accept that ‘we are not safe, until we are all safe’. It would be devastating to see a scenario similar to India play out in Africa due to insufficient vaccination.
Read more:
TRIPS waiver: US support is a major step but no guarantee of COVID-19 vaccine equity
The second response for policymakers is a more long term strategy. Certainly, the data from the study suggest that regulations are needed for minimum resource requirements for critical care provision in Africa. The study shows that there is a need for a substantial increase in resources needed to provide an acceptable quality of critical care in Africa.
Lastly, we are very aware that the situation is more dire than the study shows. This is for two reasons.
The first is that only 10 countries out of 40 that were initially invited took part in the survey. It’s likely that the countries that did’t take part didn’t have the capacity to participate because of the demand on their clinical service delivery during the pandemic. And it’s likely that these sites may have worse outcomes than reported in the study.
Secondly, the participating hospitals were predominated by university and tertiary hospitals. These are better resourced than critical care units in hospitals of a lower level. They are, therefore, in a better position to provide more comprehensive care, with possibly better outcomes than non-participating sites.
In conclusion, outcomes for critically ill Covid-19 patients in Africa are poorer than any other region in the world. This is driven by resource-poor facilities. As long as the population of Africa remains unvaccinated, this has the potential for a catastrophic loss of life in Africa.![]()
Bruce M Biccard, Professor and Second Chair at Groote Schuur Hospital , University of Cape Town
This article is republished from The Conversation under a Creative Commons license. Read the original article.